Nursing staff said they were too busy to give residents water, showers. One of their residents died a month later.
A grandmother's family was awarded $6 million after she died at a Gwinnett County nursing home with a history of violations.

This past March, a jury awarded $6 million to the family of a grandmother who died at a Gwinnett County nursing home with a history of violations. The case centered on a growing problem in the long-term care industry, leading some to believe it contributed to the woman’s death. President Biden believes his plan will help.
Dubose's Death
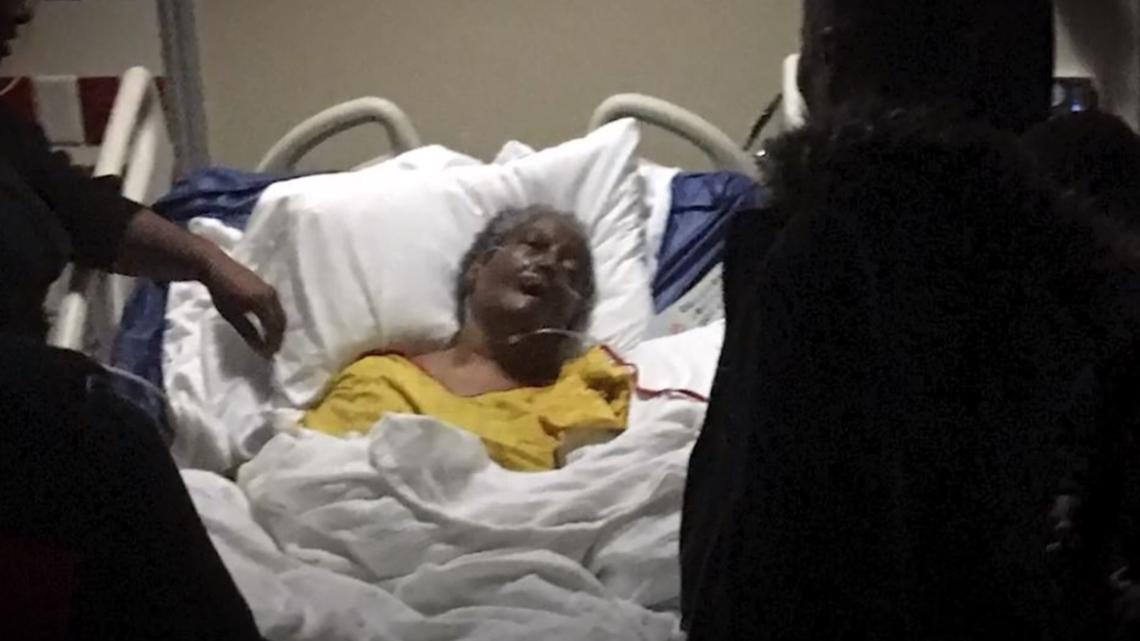
Lucille Debose died in 2016 from complications of an untreated pressure wound 33 days after her family admitted her to the Life Care Center of Lawrenceville following a stroke. Dubose was also diagnosed with dementia.
Pressure wounds are injuries to the skin and underlying tissue after prolonged pressure. It can be prevented by regularly moving patients.
By the time a doctor discovered a sore, the lawsuit claims a hole the size of a hand had developed on the 77-year-old’s lower back. It was so deep that a doctor could see the bone.
“She was hurt for 10 days, and no one did anything,” Michelle McKinney, Dubose’s daughter, said.


An 11Alive investigation uncovered that staffing shortages at the facility likely contributed to Debose’s death. It’s a claim not made by the family but by at least three former Life Care employees who worked at the facility and treated Dubose, discovered through court depositions.
“It was not sufficient staff. They would often ask you to do doubles,” Lakeisha Raymond, a former Life Care certified nursing assistant, said.
“Unfortunately, the staffing issue was an issue,” Tabitha Freeman, a former Life Care nurse who also treated Dubose. “If you don't have the staffing to provide the care, then the patient loses out.”
“They were understaffed,” Nikki Smith, another former Life Care nurse who worked at the Lawrenceville facility during the time, said.


During the deposition with Raymond, attorneys asked her whether staffing shortages impacted patient care. Raymond said she and other CNAs were often too busy to give residents water.
"There just wasn’t time for that," he said.
The long-time CNA also said staff often did not have enough time to give residents showers, and they would falsify records to conceal it.
“We would just mark that they had the showers,” Raymond said.
Life Care has appealed the jury’s verdict. They also declined 11Alive’s request for an interview.
In a prepared statement, Life Care claims the facility “was never understaffed during Ms. Dubose’s residency.” The company said the facility “had twice the Georgia state-required staffing level for nursing hours per patient per day.”
It also called the former employees 'disgruntled' and said two of three were fired.
Life Care said the third employee was once engaged to McKinney’s son, questioning her credibility. Court records show the employee was a witness for the company, not the family.


The nurses were not the only employees concerned with staffing shortages. According to a company email obtained through court records, a hiring manager recognized the problem, too.
“When I started, I became aware of the very high turnover at the facility,” said Linda John, the facility’s staff development coordinator at the time.
John’s email to Life Care’s human resource office also announced her resignation, saying she was leaving because the facility’s director of nursing caused her 'mental anguish.'
For months leading up to Debose’s death, company emails show a corporate vice president repeatedly asked facility operators to limit overtime and the hours staff worked based on a formula the company used to reduce labor costs.
“We are going to need to find some opportunities for labor reduction in just about every one of our buildings,” said the vice president in an August 2016 email to managers. “We have to really focus on actual census vs. labor daily and where we can reduce.”
The Problem and The Proposal
Since Dubose’s death, staffing shortages in the long-term care industry have reached a crisis.
A new study by Seniorly, released in April, shows understaffed long-term care facilities in the U.S. doubled during the pandemic. That’s a 7.2% increase since 2020. Georgia ranks the 13th in the country, with 28.3% of facilities understaffed.
The Georgia Health Care Association and the Georgia Center for Assisted Living say the problem is pervasive across all member facilities.
“Prior to the pandemic, nursing homes were already experiencing workforce shortages due to chronic underfunding and an inability to pay competitive wages. COVID-19 has exacerbated these challenges, and centers continue to face a workforce crisis,” said Devon Barill, the director of communications for both organizations.
Leading Age, a national organization representing 5,000 nonprofit long-term care providers, estimates that 400,000 people left the sector during the pandemic, and most of them will not come back.
“So we're really facing an enormous gap, in terms of the number of staff we need and the number of staff who are available and willing to work,” said Katie Sloan, the organization’s CEO.


Earlier this year, President Biden vowed to improve nursing home care.
“As Wall Street firms take over more nursing homes, the quality in those homes has gone down and costs have gone up. That ends on my watch,” said Biden during his State of Union speech in March. “Medicare is going to set higher standards for nursing homes and make sure loved ones get the care they deserve and they expect and they will be looked at closely.”
In February, his administration outlined a long list of proposals to do it. One includes establishing a minimum nursing home staffing requirement. The federal government would fund it.
Over the next year, the Centers for Medicare & Medicaid Services is expected to conduct a study to determine the level and type of staffing needed.
Sloan believes a study is needed, but she said the president’s proposal alone wouldn’t fix the problem.
“I think the challenge for us right now is to come up with staffing ratios that are mandated, but we don't have the people there to fill those jobs. And we're going to be back to the same place we are now, but we'll be punished for not having adequate staff,” said Sloan.
Leading Age believes raising the Medicaid reimbursement rate for long-term care providers is key to improving staffing.
“Medicaid rates simply haven't kept up with the cost of care. And that deflates what we can pay our staff. So if you've got a $100 a day gap in what Medicaid pays and the cost of providing quality care, it's unsustainable. We can't simply increase wages,” said Sloan.
Life Care Center of Lawrenceville is not a member of Sloan’s organization.
Atlanta Attorney Lance Lourie represents the Dubose family. He believes the nursing home industry does have enough money to fix staffing problems, but it chooses profits over patient care.
“There's plenty of money there to provide good care and they're not going to convince me otherwise because I've just been doing this too long,” said Lourie.
History of Violations
The Georgia Department of Community Health (DCH) cited Life Care Center of Lawrenceville for numerous violations related to Dubose’s treatment.
“The facility failed to notify the physician of a newly developed pressure ulcer and failed to obtain treatment orders for 10 days for [Dubose],” wrote a state investigator in inspection records in February 2017.
“There was not any evidence of any documentation that any treatment orders were obtained or that [Dubose] was provided wound treatment for the open area to the resident’s sacrum,” said the inspection, which also noted staff’s inaction put Dubose in immediate jeopardy.
The 125-bed facility, built-in in 1999, has a history of violations that spans years before and after Dubose’s death.

In 2005, Life Care agreed to pay $2.5 million to the federal government after five whistleblowers alleged the Gwinnett County center failed to adequately care for patients, resulting in several residents' premature deaths.
According to a press release issued by the U.S. Attorney’s Office for the Northern District of Georgia, the whistleblowers also alleged the facility suffered from severe staffing shortages.
"The settlement represents the largest recovery against a single skilled nursing facility under the False Claims Act based on a failure of care case to date," said Peter Keisler, Assistant Attorney General for the Civil Division, on December 22, 2005.
This past February, a DCH inspection identified more violations, including another example of poor pressure wound care. According to inspectors, the state identified:
- The facility failed to ensure that a resident who entered the facility with a pressure ulcer received care and services to promote healing.
- The facility failed to develop an interdisciplinary and resident-centered plan of care to manage chronic pain for at least one resident.
- The facility failed to ensure that staff followed transmission-based precautions for COVID-19 for two residents.
- The facility failed to ensure resident wishes were correctly entered into orders to reflect the residents' preferred code status.
Read the full 32-page health survey from DCH below:
MORE 11ALIVE INVESTIGATIONS:

